You wake up exhausted even after eight hours in bed. Your jaw is clenched, your neck muscles feel like concrete, and you cannot seem to shake off a lingering brain fog. You might schedule doctor appointments or scroll through medical websites searching for a hidden illness. More often than not, these are the direct physical manifestations of a chronically overworked nervous system. When your biological alarm gets stuck in the "on" position, mental overload transforms into physiological damage.
The Biological Trigger: What Does Stress Do to Your Brain?
Stress is not merely an emotion or a psychological state. It is a highly coordinated chemical reaction initiated by your brain. To understand how mental pressure dismantles physical health, you must first answer a foundational question: exactly what does stress do to your brain?
The process begins in the amygdala, the area of your brain responsible for emotional processing and threat detection. When you perceive a threat—whether it is an approaching car running a red light or an impending deadline at work—the amygdala instantly sends a distress signal to the hypothalamus.
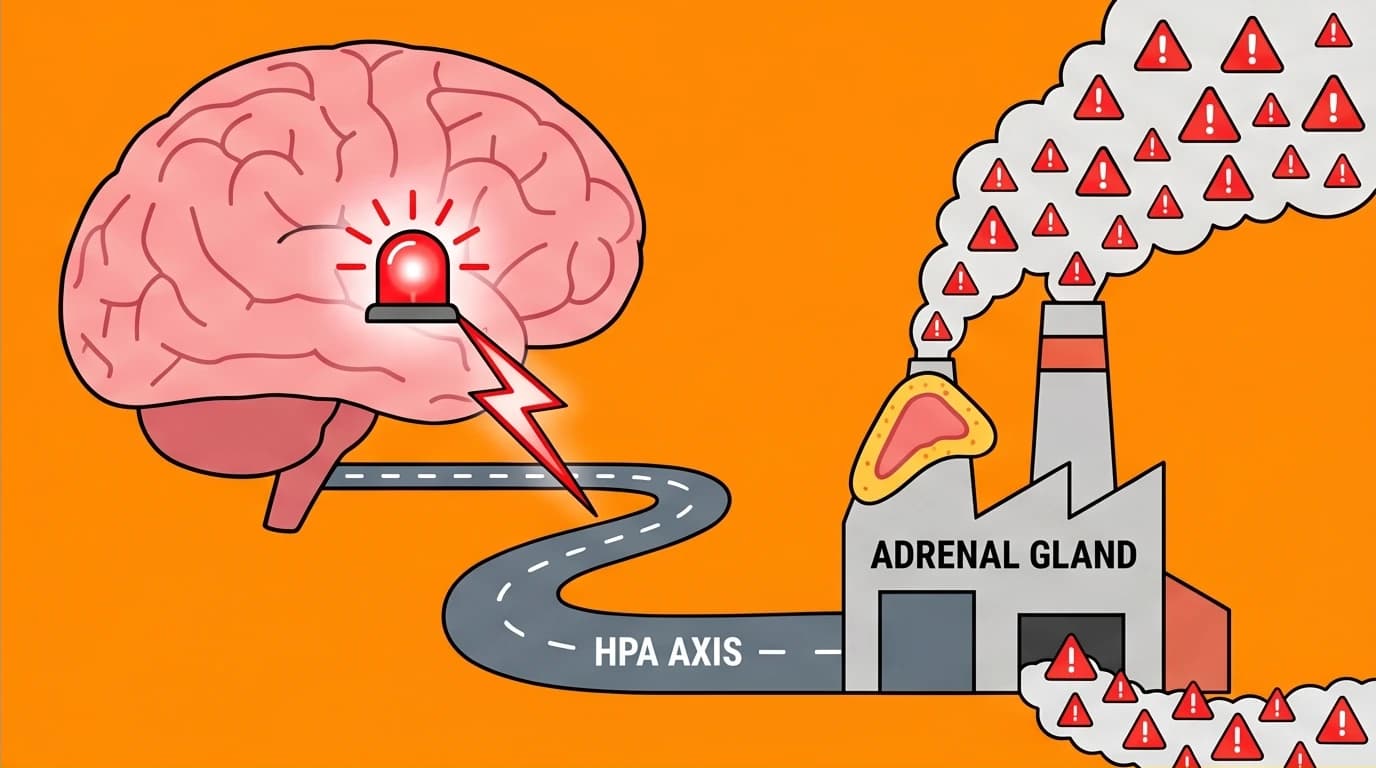
The hypothalamus functions as the command center for your autonomic nervous system. It communicates with the rest of your body through the sympathetic nervous system, triggering the "fight-or-flight" response. This pathway, known as the HPA (hypothalamic-pituitary-adrenal) axis, acts as the biochemical highway for stress.
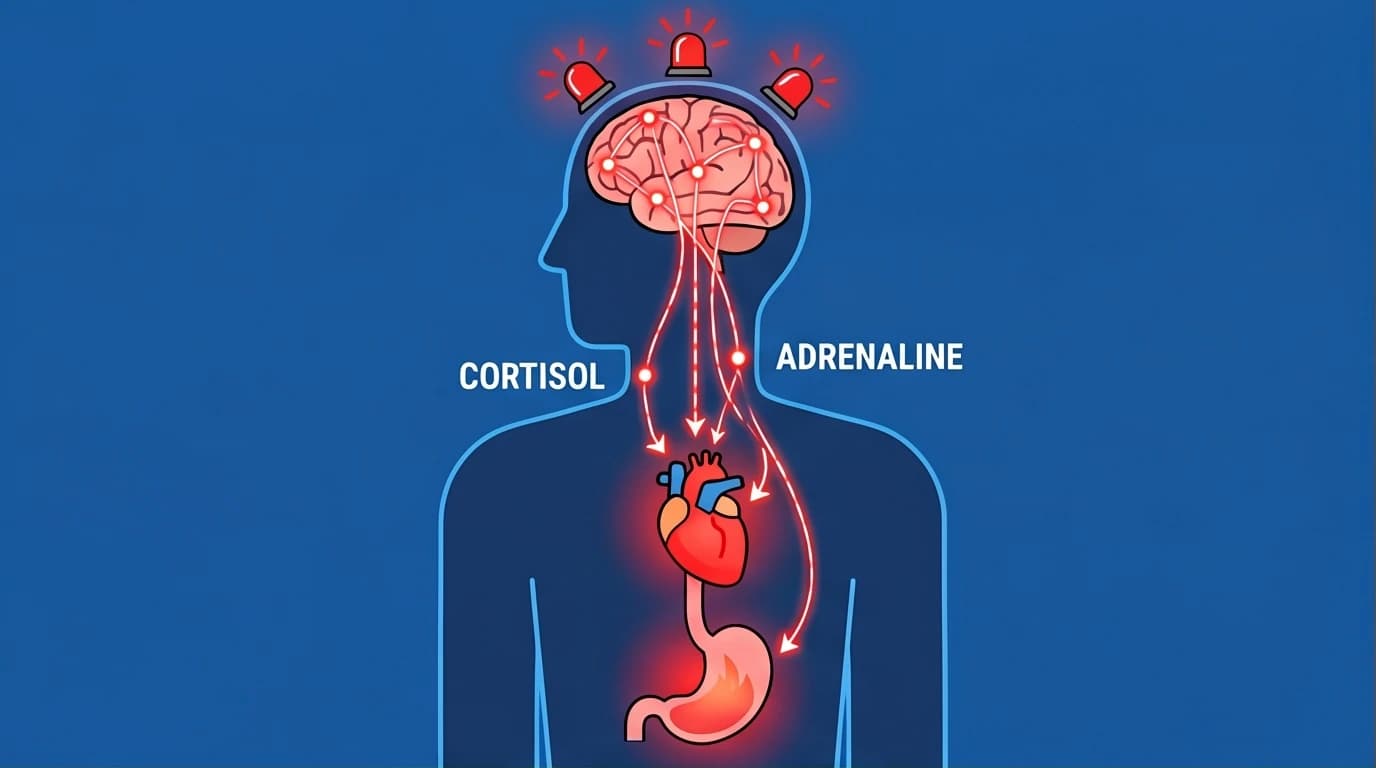
Within milliseconds, your adrenal glands pump epinephrine (adrenaline) into your bloodstream. Your heart rate accelerates. Your blood pressure spikes. Your breathing becomes rapid to force more oxygen into your lungs and brain.
If the perceived threat does not subside, the HPA axis releases cortisol, the body’s primary stress hormone. Cortisol keeps the system on high alert. It alters immune system responses, suppresses the digestive system, and impacts the reproductive system. Once the threat passes, cortisol levels drop, and the parasympathetic nervous system (the "rest and digest" network) brings your body back to baseline. However, when the psychological pressure is constant, the alarm never turns off.
Structural Brain Changes
Over time, high levels of cortisol literally reshape brain architecture. Chronic stress shrinks the prefrontal cortex, the area responsible for memory, learning, and executive function. Simultaneously, it increases the size of the amygdala, making your brain even more hyper-reactive to future stressors. This neuroplastic shift explains why chronically stressed individuals often struggle with forgetfulness, lack of focus, and sudden outbursts of anger.
Since many of these modern stressors originate from our professional lives, understanding how to handle that specific environment is key. For a deeper look into dealing with job-related pressure, these strategies can make a significant difference.
If you find yourself fascinated—or perhaps a bit alarmed—by how your body chemically reacts to modern anxiety, there is a phenomenal resource to dive into next. To truly understand why human beings suffer from chronic stress while wild animals easily shake off life-or-death encounters, you might want to explore the biological mechanics further. This foundational read provides a brilliant, often humorous look at how our cardiovascular and neurological systems handle constant pressure, making it highly recommended for anyone looking to make sense of their physiological stress response.

Why Zebras Don't Get Ulcers
Robert M. Sapolsky
Identifying the Physical Symptoms of Stress
Because stress hijacks the central nervous system, its impact cascades through every major organ group. Many people mistake these indicators for distinct illnesses, failing to realize they are interconnected physical symptoms of stress.
The Musculoskeletal System
Under acute stress, your muscles instantly tense up to protect themselves from injury. This is a reflex action. When stress becomes chronic, muscles remain in a constant state of guarded tightness. This unrelenting tension restricts blood flow and leads to chronic pain conditions. Tension headaches, severe migraines, tight shoulders, and lower back pain are often the direct results of sustained muscular contraction.
The Respiratory and Cardiovascular Systems
Stress causes you to breathe harder and faster. For individuals with preexisting respiratory conditions like asthma or chronic obstructive pulmonary disease (COPD), stress can trigger life-threatening acute attacks.
Simultaneously, your heart pumps faster to distribute oxygen-rich blood to major muscle groups. Blood vessels constrict. While this helps you physically run away from danger, experiencing this at your desk day after day places massive wear and tear on your blood vessels. This continuous strain forces your heart to work overtime, significantly elevating your resting blood pressure.
The Gastrointestinal System
Your gut and brain maintain continuous communication through the vagus nerve. When the brain detects stress, it redirects energy away from digestion to prioritize muscle function and immediate survival.
This disruption causes a variety of immediate digestive issues. The rush of hormones can trigger acid reflux, nausea, or severe stomachaches. Stress also heavily alters the speed at which food moves through your body, leading directly to diarrhea or constipation. Furthermore, cortisol disrupts the delicate balance of your gut microbiome, increasing intestinal permeability (often referred to as leaky gut) and triggering systemic inflammation.
The complex communication network between your brain and your digestive tract often holds the key to unexplained physical symptoms. If you regularly experience bloating, indigestion, or stomachaches during highly stressful weeks, you are likely feeling the direct impact of cortisol on your microbiome. For those who want to learn exactly how to heal this biological pathway, exploring the science behind your digestive system's nervous network can be completely life-changing. Understanding this intricate link will empower you to restore your gut health and, by extension, your mental clarity.

The Mind-Gut Connection
Emeran Maye
It can be a lot to take in, especially when you're already feeling the physical drain of stress. If sitting down with a dense science book feels like too much right now, you can learn the core concepts in a more accessible way.
Understand the science behind stress and health by listening to summaries of books like The Mind-Gut Connection in short, easy-to-digest audio sessions.

Download LeapAhead App now
The Long Term Effects of Chronic Stress
Human biology is incredibly resilient to acute, short-term stress. You get scared, your heart races, you recover. But the human body is categorically incapable of managing constant, low-grade daily stress without suffering structural damage. The long term effects of chronic stress act as a slow-motion wrecking ball on your vital organs.
Cardiovascular Disease
Decades of continuous heart rate spikes and elevated blood pressure eventually damage the lining of blood vessels. This vascular inflammation makes it easier for cholesterol plaque to build up. Chronic stress is a primary driver of hypertension, significantly increasing the likelihood of heart attacks and strokes.
Decades of continuous heart rate spikes and elevated blood pressure eventually damage the lining of blood vessels. This vascular inflammation makes it easier for cholesterol plaque to build up. Chronic stress is a primary driver of hypertension, significantly increasing the likelihood of heart attacks and strokes.
Metabolic Syndrome and Type 2 Diabetes
Cortisol forces your liver to release extra glucose into your bloodstream to provide fast energy. When you do not physically burn off that glucose (because you are sitting in an office or a car), your pancreas must pump out insulin to bring blood sugar levels down. Over time, this constant cycle leads to insulin resistance, paving the way for Type 2 diabetes. Additionally, cortisol specifically promotes the storage of visceral fat around your abdomen, a key indicator of metabolic syndrome.
Cortisol forces your liver to release extra glucose into your bloodstream to provide fast energy. When you do not physically burn off that glucose (because you are sitting in an office or a car), your pancreas must pump out insulin to bring blood sugar levels down. Over time, this constant cycle leads to insulin resistance, paving the way for Type 2 diabetes. Additionally, cortisol specifically promotes the storage of visceral fat around your abdomen, a key indicator of metabolic syndrome.
Immune System Suppression
While acute stress briefly stimulates the immune system to prepare for potential physical wounds, chronic stress severely suppresses it. Sustained cortisol presence reduces the production of lymphocytes, the white blood cells necessary for fighting off viruses and bacteria. You become significantly more susceptible to common colds, the flu, and infections. Furthermore, chronic stress exacerbates autoimmune diseases, causing flare-ups in conditions like rheumatoid arthritis, lupus, and psoriasis.
While acute stress briefly stimulates the immune system to prepare for potential physical wounds, chronic stress severely suppresses it. Sustained cortisol presence reduces the production of lymphocytes, the white blood cells necessary for fighting off viruses and bacteria. You become significantly more susceptible to common colds, the flu, and infections. Furthermore, chronic stress exacerbates autoimmune diseases, causing flare-ups in conditions like rheumatoid arthritis, lupus, and psoriasis.
Accelerated Cellular Aging
At a genetic level, chronic stress shortens telomeres—the protective caps at the ends of your chromosomes. As telomeres shorten, cells age faster and die off quicker. This accelerates the physical aging process, making you look older and causing your biological age to surpass your chronological age.
At a genetic level, chronic stress shortens telomeres—the protective caps at the ends of your chromosomes. As telomeres shorten, cells age faster and die off quicker. This accelerates the physical aging process, making you look older and causing your biological age to surpass your chronological age.
Reading about these consequences can be alarming. The most effective way to protect your long-term health is to proactively change your relationship with stress and develop the mental frameworks to handle pressure more effectively.
It can be sobering to realize how deeply suppressed emotions and relentless mental overload translate into tangible, long-term diseases. When you ignore the warning signs of chronic stress, your physical biology eventually forces you to pay attention, often manifesting as severe autoimmune or metabolic conditions. If you are struggling to set boundaries or constantly pushing yourself past the point of exhaustion, learning how emotional stress converts into physical illness is a crucial step toward recovery. This eye-opening perspective might be exactly what you need to finally prioritize your health.

When the Body Says No
Gabor Mate, MD

Recognizing the Warning Signs of Stress
Intervention requires awareness. Do not wait for a major cardiovascular event or a severe panic attack to force a lifestyle change. Your body constantly transmits warning signs of stress. Identifying these markers early allows you to intercept the biological damage before it becomes permanent.
Physiological Markers
- Sleep Disruption: Difficulty falling asleep, waking up constantly in the middle of the night, or feeling unrefreshed after a full night’s sleep. High nighttime cortisol prevents the brain from entering deep, restorative sleep cycles.
- Unexplained Weight Fluctuations: Sudden weight gain (particularly belly fat) despite no major dietary changes, driven by stress-induced cortisol and insulin spikes.
- Frequent Illness: Catching every bug circulating through your office or household due to a depressed immune response.
- Hair Loss: A condition called telogen effluvium, where severe stress pushes hair follicles into a resting phase, causing hair to fall out in clumps during brushing or washing.
Cognitive and Emotional Markers
- Persistent Brain Fog: An inability to concentrate, forgetting simple tasks, or struggling to organize your thoughts during meetings.
- Emotional Volatility: A drastically shortened temper. Snapping at family members or coworkers over minor inconveniences that previously would not bother you.
- Apathy and Burnout: A profound loss of motivation or a feeling of detachment from activities you usually enjoy.
Behavioral Markers
- Changes in Appetite: Either skipping meals entirely because your stomach is tied in knots, or compulsively binge-eating high-sugar, high-fat foods for a temporary dopamine hit.
- Increased Reliance on Substances: Reaching for a stiff drink every night to transition away from work mode, or drinking multiple pots of coffee just to maintain basic functioning.
- Nervous Habits: Developing physical tics like nail-biting, jaw clenching (bruxism) at night, or restless leg movements.
The effects of stress on the body are profound, measurable, and highly destructive. Recognizing that mental pressure directly dictates biological health is the first step toward reclaiming your well-being. You cannot eliminate all stress from modern American life, but by understanding its physiological mechanics, you can implement targeted recovery strategies—like rigorous exercise, deep sleep hygiene, and professional therapy—to force your nervous system back into balance.
If you are seeing these warning signs in your own life, taking action is the most important next step. For a practical overview of different ways to cope, you can start here.
Breaking the cycle of chronic stress requires more than just a weekend getaway or a bubble bath; it demands a strategic approach to completing your body's biological stress cycle. If you are recognizing these warning signs in your own behavior and feeling overwhelmed by the sheer weight of your daily responsibilities, there are incredibly effective ways to bounce back. By learning actionable, science-backed techniques to release trapped physiological tension, you can finally find relief. This powerful guide is a must-read for anyone ready to process their exhaustion and reclaim a joyful, balanced life.

Burnout
Emily Nagoski, Ph.D., Amelia Nagoski, DMA
With so many powerful books recommended, it's easy to feel like you have a mountain of reading to do. If finding the time and energy to get through them all feels daunting, you can start by absorbing their core lessons in a more manageable format.
Absorb key lessons from bestselling wellness books in 15-minute audio sessions, making it easier to build a learning habit even on your most stressful days.

Download LeapAhead App now
FAQ
Can stress make you physically sick?
Yes. Stress is not just a mental state; it triggers real biological changes. Chronic stress heavily suppresses your immune system by reducing lymphocyte production, making it significantly harder for your body to fight off viruses and bacteria. It also causes systemic inflammation that can trigger or worsen physical illnesses like heart disease, asthma, and gastrointestinal disorders.
Yes. Stress is not just a mental state; it triggers real biological changes. Chronic stress heavily suppresses your immune system by reducing lymphocyte production, making it significantly harder for your body to fight off viruses and bacteria. It also causes systemic inflammation that can trigger or worsen physical illnesses like heart disease, asthma, and gastrointestinal disorders.
How long does it take for the body to recover from chronic stress?
Recovery timelines vary based on how long you have been under chronic stress and the severity of the symptoms. Acute physical symptoms like muscle tension or elevated heart rate can subside within hours of a stressor passing. However, reversing chronic damage—such as repairing adrenal fatigue, lowering resting cortisol levels, and restoring a healthy gut microbiome—can take several months of consistent lifestyle interventions, proper sleep, and active stress management.
Recovery timelines vary based on how long you have been under chronic stress and the severity of the symptoms. Acute physical symptoms like muscle tension or elevated heart rate can subside within hours of a stressor passing. However, reversing chronic damage—such as repairing adrenal fatigue, lowering resting cortisol levels, and restoring a healthy gut microbiome—can take several months of consistent lifestyle interventions, proper sleep, and active stress management.
Does stress cause weight gain?
Yes. When you are chronically stressed, your body produces high levels of cortisol. Cortisol not only increases your appetite and cravings for high-calorie, sugary foods, but it also alters your metabolism. It signals your body to store excess energy as visceral fat, particularly around the abdomen, which is highly resistant to traditional diet and exercise.
Yes. When you are chronically stressed, your body produces high levels of cortisol. Cortisol not only increases your appetite and cravings for high-calorie, sugary foods, but it also alters your metabolism. It signals your body to store excess energy as visceral fat, particularly around the abdomen, which is highly resistant to traditional diet and exercise.
Is hair loss from stress permanent?
Typically, no. Stress-induced hair loss, medically known as telogen effluvium, occurs when a shock to your system pushes a large number of hair follicles into a resting phase. The hair usually falls out a few months after the stressful event. Once the underlying stress is managed and cortisol levels return to normal, the hair follicles typically shift back into the growth phase, and the hair will grow back over the following six to nine months.
Typically, no. Stress-induced hair loss, medically known as telogen effluvium, occurs when a shock to your system pushes a large number of hair follicles into a resting phase. The hair usually falls out a few months after the stressful event. Once the underlying stress is managed and cortisol levels return to normal, the hair follicles typically shift back into the growth phase, and the hair will grow back over the following six to nine months.